Fever

Raised temperature (above 38°C or 100°F) is a common accompaniment of respiratory and other infections, and doctors agree that this is not usually serious. (However do heed the advice below, and read the Safety Notice on the Introduction page). Fever is a sign that the body is defending itself: raising temperature activates white blood cells and other defences.
Unless there are serious complications antibiotics or other prescriptions are not appropriate, and self-administered aspirin is considered no longer safe especially for children.
Paracetemol or ibuprofen are often used by patients or parents to control fever symptoms. However there are old skills of fever management that can help. Proper fever management can even make good of an uncomfortable experience by priming the body’s immune defences for long-term protection and preventing future viral infections. These old techniques have largely been lost and parents especially can easily be alarmed by the situation. The following is simple home advice to manage a fever safely.
First, check the NHS websites for up-to-date information for managing fevers in children and adults. In particular note complicating conditions that mean you will need to call in professional help.
Second, note these reasons to seek medical attention:
If looking after a child with fever seek professional attention if any of the following conditions exist:
- is under three months old and has a temperature of 38C (101F) or above
- is between three and six months old and has a temperature of 39C (102F) or above;
- otherwise if the temperature climbs to 40°C (104°F) or higher.
- the fever has lasted more than five days.
- There is a rash which does not disappear when pressed under a glass
- there are other signs of being unwell, such as persistent vomiting, refusal to feed, floppiness or drowsiness.
- You are already on strong or life-saving medication or have a prior severe medical condition.
- Your temperature climbs to 40°C (104°F) or higher.
- The fever has lasted more than three days.
- You have chest pain or trouble breathing
- You have severe thirst or reduced urine output
- You have previously fainted or feel like you are about to faint.
- You experience confusion or excessive drowsiness.
- Your symptoms have worsened or you notice new symptoms
- Your fever followed recent foreign travel.
- Regularly check the temperature with a thermometer (by mouth in adults or grown children; in armpit or with an ear thermometer in babies and children: forehead strips are not accurate).
- Then check whether the sufferer feels hot or cold.
If feeling cold the temperature you record is still going up – you need to be more alert and take more precautions; keep the sufferer warm;
If feeling hot the temperature you record is coming down you can be more relaxed and allow the sufferer to remove clothes if needed though not enough to get a second chill.
- Always make sure the sufferer is taking enough fluid to prevent dehydration.
- Food is not urgent – when hungry go for easy-to-digest foods like soups and stews.
- Ensure plenty of rest and quiet – it often helps to draw curtains in the room to reduce light.
- Allow plenty of time for full recovery when the fever has broken: a day or so at least.
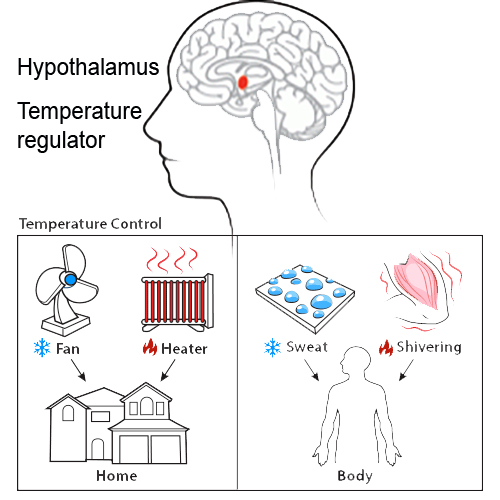
You can think of body temperature being set by a ‘thermostat’ (it’s actually in the hypothalamus in the brain). Think what happens when you set the thermostat higher for central heating in a building: the boilers fire up and heat is pumped out. Its similar in the body – in this case the muscles and metabolism generate heat (see diagram).
Infections can set the body thermostat higher.
So for a while after infection the body temperature is lower than the new setting, and it needs to warm up. This is the ‘chills’ stage of a fever: you feel cold: you shiver (to generate heat from muscle activity), the circulation is closed down at the surface, and you look for ways to warm up. At this stage your body temperature is going up.
When the fever peaks the reverse happens: the ‘thermostat’ setting is lowered and the body temperature is now higher: you feel hot, and to cool down start sweating, drinking cold drinks and so on. At this stage your body temperature is going down.
